Anatomy/Cardiovascular System
The cardiovascular system, also known as the circulatory system, is a topic in Anatomy and Physiology. It was tested in both 2015, 2019, and 2024.
Overview
| Competition Level | Health Concepts |
|---|---|
| Regional/State |
|
| National |
|
Functions
- Transportation: The cardiovascular system transports nutrients, oxygen, and hormones to the cells and metabolic wastes like carbon dioxide away from the cells.
- Protection: Circulating throughout the blood are leukocytes (white blood cells) and other defenses against antigens.
- Regulation: Homeostasis is maintained in the body through regulation of pH, temperature, and water content of cells.
Formulas
To determine the values for these calculations, data like blood pressure and heart rate must be measured with a sphygmomanometer. When this is being used, a doctor puts a cuff around the arm and pumps it up, exerting pressure and cutting off blood flow. As the pressure is being released, the blood starts to flow again, and doctors listen to these sounds to measure the systolic pressure and diastolic pressure. Heart rate can be measured by counting the number of beats felt in a minute and doesn't require any machinery.
- Heart Rate (HR): Number of heartbeats per minute
- Stroke Volume (SV): Amount of blood pumped out of the heart in one beat: Stroke Volume = End Diastolic Volume - End Systolic Volume (SV = EDV - ESV)
- Pulse Pressure (PP): The difference between systolic pressure (SP) and diastolic pressure (DP) - Pulse Pressure = Systolic Pressure - Diastolic Pressure (PP = SP - DP)
- Cardiac Output (CO): Amount of blood pumped out of the heart in one minute - Cardiac Output = Heart Rate x Stroke Volume (CO = HR x SV)
- Mean Arterial Pressure (MAP): The average pressure in the arteries during one cardiac cycle - Mean Arterial Pressure = 2/3 Diastolic Pressure + 1/3 Systolic Pressure (MAP = 2/3 DP + 1/3 SP) OR Mean Arterial Pressure = Diastolic Pressure + 1/3 Pulse Pressure (MAP = DP + 1/3 PP)
The Heart
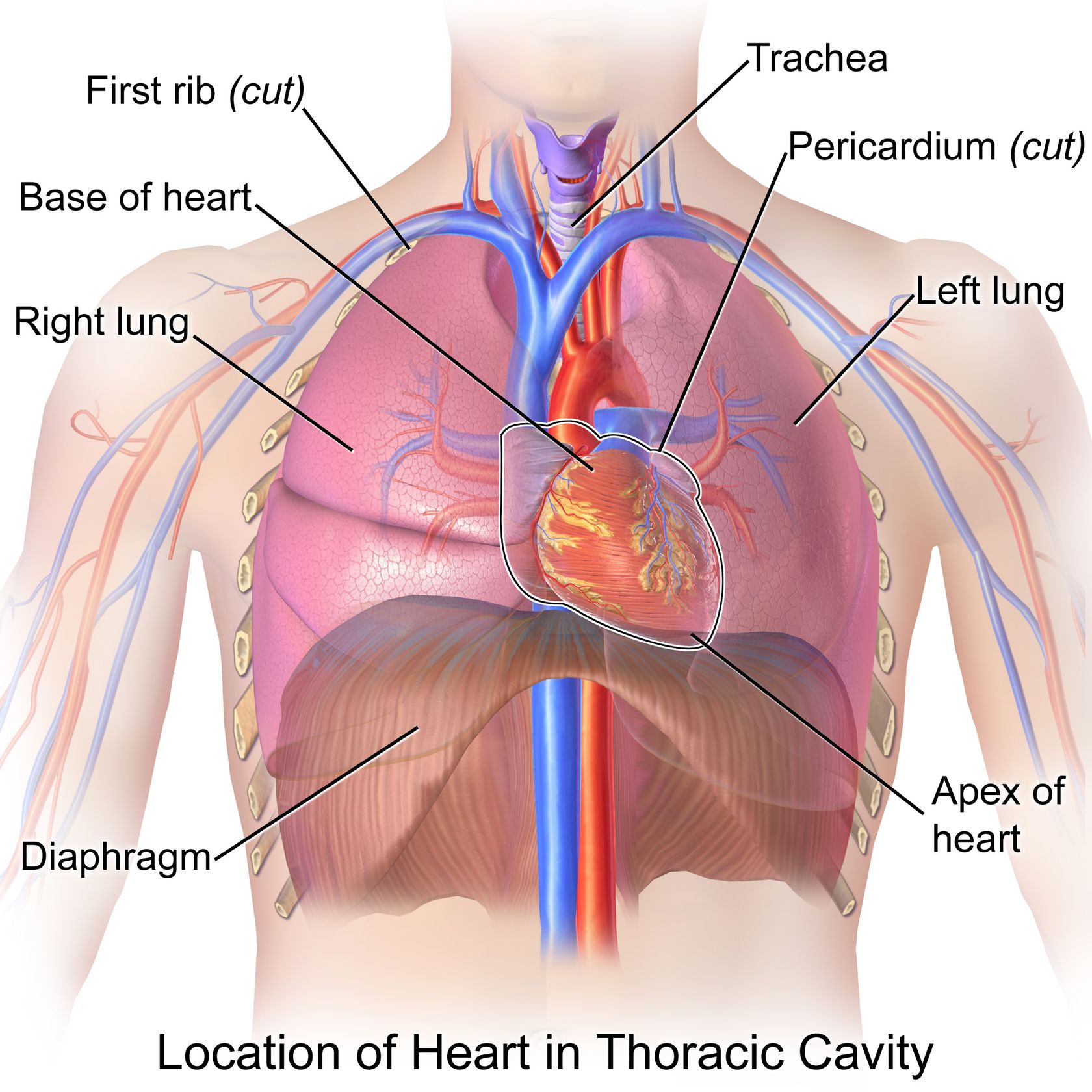
The heart is the main organ of the cardiovascular system. It is a muscular organ about the size of one's fist and weighs between 7-15 ounces. It acts as a pump and propels blood through the blood vessels. The average heart beats about 100,000 times a day, circulating about 2,000 gallons of blood through about 60,000 miles of blood vessels. An adult has, on average, 5 to 6 quarts of blood. The average adult resting heart rate is 72 bpm (beats per minute).
The heart is located in the middle of the thorax with part of it offset slightly to the left. It is underneath the sternum (breastbone) and is surrounded by the lungs. It sits on the diaphragm and is protected by the ribcage. It is inside of a sac known as the pericardium.
In general, the left side of the heart (which is located on the right side in a diagram) is the pump for the systemic circuit, which takes blood to and from the body. The right side of the heart (which is located on the left in a diagram), is the pump for the pulmonary circuit, which takes blood to and from the lungs.
The sound of the heartbeat can be described as "lubb-dupp". The first sound, or the "lubb", comes from the closing of the atrioventricular valves, which are the tricuspid and mitral (bicuspid) valves. The second sound, which is the "dupp", comes from the closing of the other two valves (semilunar valves), which are the aortic and pulmonary valves. After the dupp should be a small pause before the lubb comes again.
Inside the heart are four chambers, two superior atria (left and right) and two inferior ventricles (left and right). The atria are areas under low pressure while the ventricles are areas under high pressure. The left side of the heart is separated from the right side of the heart by a wall of muscle known as the septum. As a general rule, ventricles are more muscular than atria because they have to pump blood to another location outside of the heart. The left ventricle is the most muscular chamber of the heart. For the right ventricle, this location is the lungs while for the left ventricle, this location is the rest of the body via the aorta. There are also four valves inside the heart: the tricuspid valve, the pulmonary valve, the mitral (bicuspid) valve, and the aortic valve. The purpose of the valves is to prevent backflow of blood back into the chamber that it came from.
Main Parts in Order of Blood Flow (also includes vessels leading in and out of the heart): Superior Vena Cava/Inferior Vena Cava, right atrium, tricuspid valve, right ventricle, pulmonary valve, pulmonary artery, pulmonary capillary bed (lungs), pulmonary veins, left atrium, bicuspid (mitral valve), left ventricle, aortic valve, aorta, arteries, arterioles, capillaries, venules, veins, Superior vena cava/inferior vena cava.
Parts of the Heart
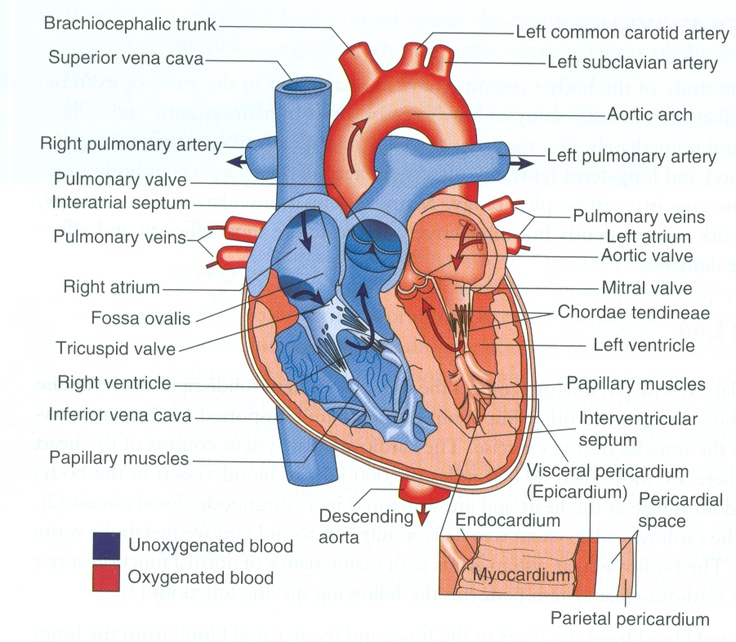
Below are the specific parts of the heart in the order that blood travels.
- Superior Vena Cava: The superior vena cava is a tube located superior to the right atrium. It brings deoxygenated blood from the upper parts of the body to the heart.
- Inferior Vena Cava: The inferior vena cava is a tube located inferior to the right atrium. It brings deoxygenated blood from the lower parts of the body to the heart.
- Right Atrium: The right atrium takes in deoxygenated blood from the superior and inferior vena cavae. It then pumps the blood through the tricuspid valve and into the right ventricle. The Sinoatrial (SA) node is located on the roof of the right atrium.
- Tricuspid Valve: The tricuspid valve, located between the right atrium and the right ventricle, prevents blood flow backward from the ventricle to the atrium. It is called the tricuspid valve because it has three leaflets.
- Right Ventricle: The right ventricle takes deoxygenated blood that has traveled through the tricuspid valve from the right atrium. It then pumps that blood through the pulmonary valve and into the pulmonary trunk.
- Pulmonary Valve: The pulmonary valve is one of the four valves of the heart, located between the right ventricle and the pulmonary trunk. Like all valves, it prevents blood from flowing backwards. The pulmonary valve is a semilunar valve, which has three cusps.
- Pulmonary Trunk: The pulmonary trunk takes in deoxygenated blood from the right ventricle and takes it to the pulmonary arteries.
- Pulmonary Arteries: The pulmonary arteries are the last part of the pulmonary circuit of the heart. They take deoxygenated blood from the pulmonary trunk and the right ventricle and take it to the lungs so that gas exchange can occur. There are two pulmonary arteries, the left and the right, which take the deoxygenated blood to the left and right lungs, respectively.
- Pulmonary Capillary Beds: The pulmonary capillary beds are located in the alveoli of the lungs. They are responsible for exchanging the carbon dioxide in the venous blood for oxygen.
- Pulmonary Veins: After gas exchange occurs at the capillary beds of the lungs, oxygenated blood goes back to the heart via the left and right pulmonary veins. They then take the blood to the left atrium.
- Left Atrium: The left atrium receives oxygenated blood from the left and right pulmonary veins. It then pumps the blood through the mitral valve and into the left ventricle.
- Mitral Valve: The mitral valve is another of the four valves of the heart. It allows blood to pass from the left atrium to the left ventricle and prevents backflow back into the atrium. It is also known as the bicuspid valve because it has two leaflets.
- Left Ventricle: The left ventricle takes in oxygenated blood from the left atrium and pumps through the aortic valve and into the aorta and then the whole body. It is the most muscular chamber of the heart due to the fact that it has to pump blood to the rest of the body.
- Aortic Valve: The aortic valve is the last of the four valves of the heart. It allows blood to pass from the left ventricle and into the aorta. It is a semilunar valve and has three cusps.
- Aorta: The aorta receives oxygenated blood from the left ventricle to take to the whole body. It is the largest artery of the body, about two centimeters in width. Three smaller arteries branch off of the aortic arch, which are the brachiocephalic artery, the left common carotid artery, and the left subclavian artery, which all supply oxygenated blood to the head and arms.
A helpful playlist of videos on the heart
Layers of Heart Tissue
The heart wall has three main layers: the endocardium, the myocardium, and the epicardium (listed from inside to outside).
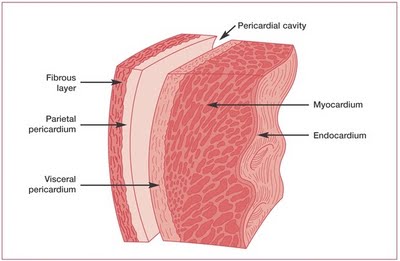
- Endocardium: The endocardium is the most interior layer of the heart wall. It is simple squamous epithelium and lines the inside of the heart's chambers. It is very smooth and is responsible for keeping the blood from sticking to the wall and potentially forming blood clots.
- Myocardium: The myocardium is the next most interior layer of the heart wall. It is the middle and muscular layer, which contains the cardiac muscle tissue. It is the thickest part of the wall and makes up most of the mass of the heart wall. The function of the myocardium is to contract and pump blood throughout the heart.
- Epicardium: The epicardium is the outermost layer. It is another name for the visceral layer of the pericardium, which is the sac that contains the heart. The epicardium is a layer of serious membrane that lubricates and protects the outside of the heart.
- Pericardium: The pericardium is the sac that the heart is inside of. Pericardium is the name for the walls and lining of the pericardial cavity. The pericardial cavity is a fluid-filled cavity with two walls on each side. The outer layer of the pericardium is the parietal layer (made of dense, fibrous connective tissue) while the inside layer is the visceral layer. The pericardium is a serous membrane that produces serous fluid to lubricate the heart. Another purpose of the pericardium is holding the heart in position and maintaining a hollow space (pericardial cavity) for the heart to expand into.
Electrical Activity of the Heart
The heart is made up of muscle tissue, consisting of muscle cells called cardiomyocytes separated by gap junctions. These gap junctions are similar to synapses in the brain, allowing for action potentials to be transmitted from one cell to the next. Action potentials are produced automatically by pacemaker tissues, creating electrical signals which move throughout the heart and cause the muscles to contract. The atria and ventricles are separated by the fibrous skeleton of the heart, so these impulses cannot be conducted directly between them. As a result, the heart has a system of specialized myocardial cells which conduct signals from the atria to the ventricles.
Parts of the Cardiac Conduction System
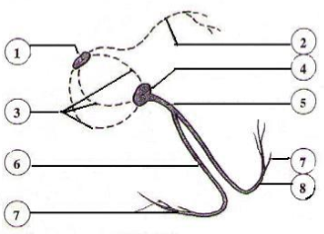
The image on the right shows the heart's electrical system with numbers in the approximate order that electricity travels (electricity travels through some parts at the same time). The labels for the numbers are as followed:
- Sinoatrial Node: Also known as the SA node, the sinoatrial node is located on the roof of the right atrium. It is the natural pacemaker of the heart.
- Intra-atrial Pathway: The intra-atrial pathway carries electricity from the sinoatrial node on the roof of the right atrium to the left atrium. This pathway leads to the Bachmann's bundle, which is a band of cardiac muscle in the left atrium which controls contraction of the left atrium.
- Internodal Pathway: The internodal pathway carries electricity from the sinoatrial node on the roof of the right atrium to the atrioventricular (AV) node located between the atria and the ventricles.
- Atrioventricular Node: Also known as the AV node, the atrioventricular node is the backup pacemaker. It is located in the interatrial septum. Its function is to slow conduction of electricity between the atria and the ventricles so blood can fill up in the ventricles and so that they do not contract at the same time.
- Bundle of His: The bundle of His is the last part of atrial conduction. It is made up of myocardial cells and is located in the ventricular wall (interventricular septum) and allows the electricity to move from the AV node and into the bundle branches in the ventricles.
- Right Bundle Branch: The right bundle branch comes off of the Bundle of His. It is one of the two branches that come off of it, with the other branch being the left bundle branch. The right bundle branch carries electricity to the right ventricle.
- Purkinje Fibers: The Purkinje fibers are located in the subendocardium layer of the heart tissue, which is the innermost layer. They distribute electrical energy to the myocardium, which is the layer of muscular tissue.
- Left Bundle Branch: The left bundle branch comes off of the Bundle of His and is the second of the two branches that come off of it. This bundle branch carries electricity to the left ventricle.
Action Potentials and Electrical Conduction of the Heart
Cells are surrounded by membranes which act to compartmentalize different areas of the body. The concentration of ions across a membrane is rarely the same between two compartments—that is, the concentration of sodium ions may be higher outside the cell than it is inside the cell, or vice versa. This difference in concentrations (concentration gradient) produces a membrane potential. A membrane potential is a measurement of how much energy it would take to move an ion from one side of the membrane to the other. Membrane potentials allow cells to act like a battery, using the energy stored in the concentration gradient to transmit signals and enact other changes in the body.
An action potential is a rapid change in membrane potential. Action potentials are produced in many different types of cells: they are used to transmit signals in the brain, and they are also responsible for muscle contractions. The heart is made up of special cardiac muscle tissue, and muscle contractions are responsible for the pumping action of the heart. Special pacemaker tissues automatically generate electrical signals by producing action potentials which tell the cardiac muscle to contract.
The sinoatrial node (SA node) is known as the primary pacemaker of the heart, as it is responsible for a majority of the heart's electrical activity. Two other regions are capable of producing action potentials of their own: the atrioventricular node (AV node) and the Purkinje fibers (also known as the subendocardial conducting network). These are known as secondary pacemakers because their activity is suppressed by the SA node, but they are still capable of producing activity in the event that the SA node is blocked.
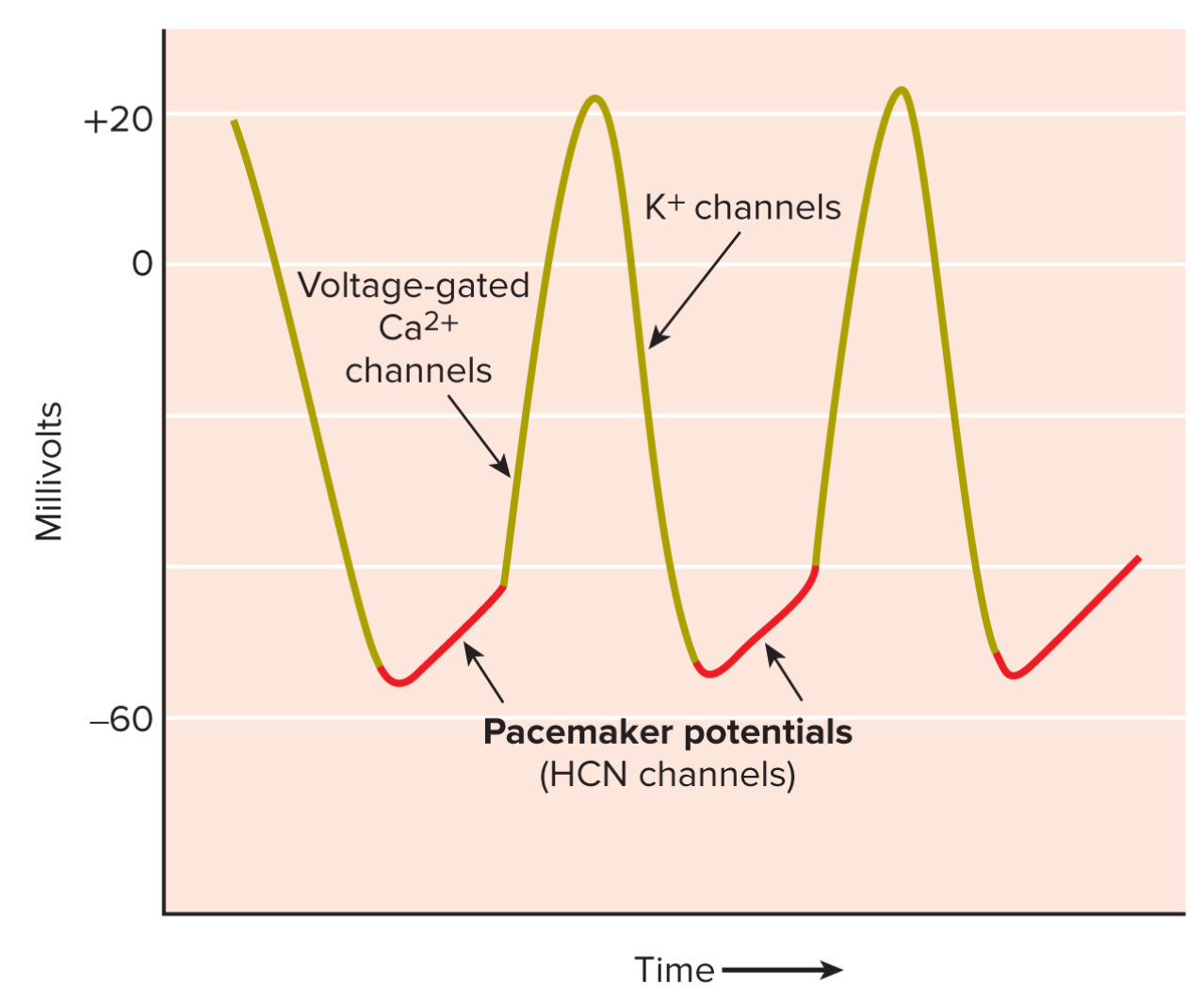
The action potential produced by pacemaker tissues is known as the pacemaker potential (also known as a diastolic depolarization, as it occurs during diastole).
The pacemaker potential is produced by ion channels in the sarcoplasmic reticulum of the cardiomyocytes. Most voltage-gated ion channels respond to a depolarization, or the inside of the cell becoming more positive/less negative relative to the outside. However, special ion channels in pacemaker cells called HCN channels respond to a hyperpolarization, which occurs when the inside of the cell becomes more negative relative to the outside. When these HCN channels open, sodium (Na+) ions enter the cell and make it more positive. This results in a depolarization event. This flow of Na+ ions into the cell is also known as the pacemaker current or "funny current", since its mechanism is so unusual.
Once the cell has reached a membrane potential of approximately -40 mV, voltage-gated Ca2+ channels in the plasma membrane open and allow calcium ions to enter the cell. This causes a sharp increase in the membrane potential, resulting in an action potential. The pacemaker cells repolarize due to the opening of voltage-gated potassium ion channels, causing the membrane potential to fall back to approximately -50 mV. The HCN channels open, and the pacemaker potential occurs once again.
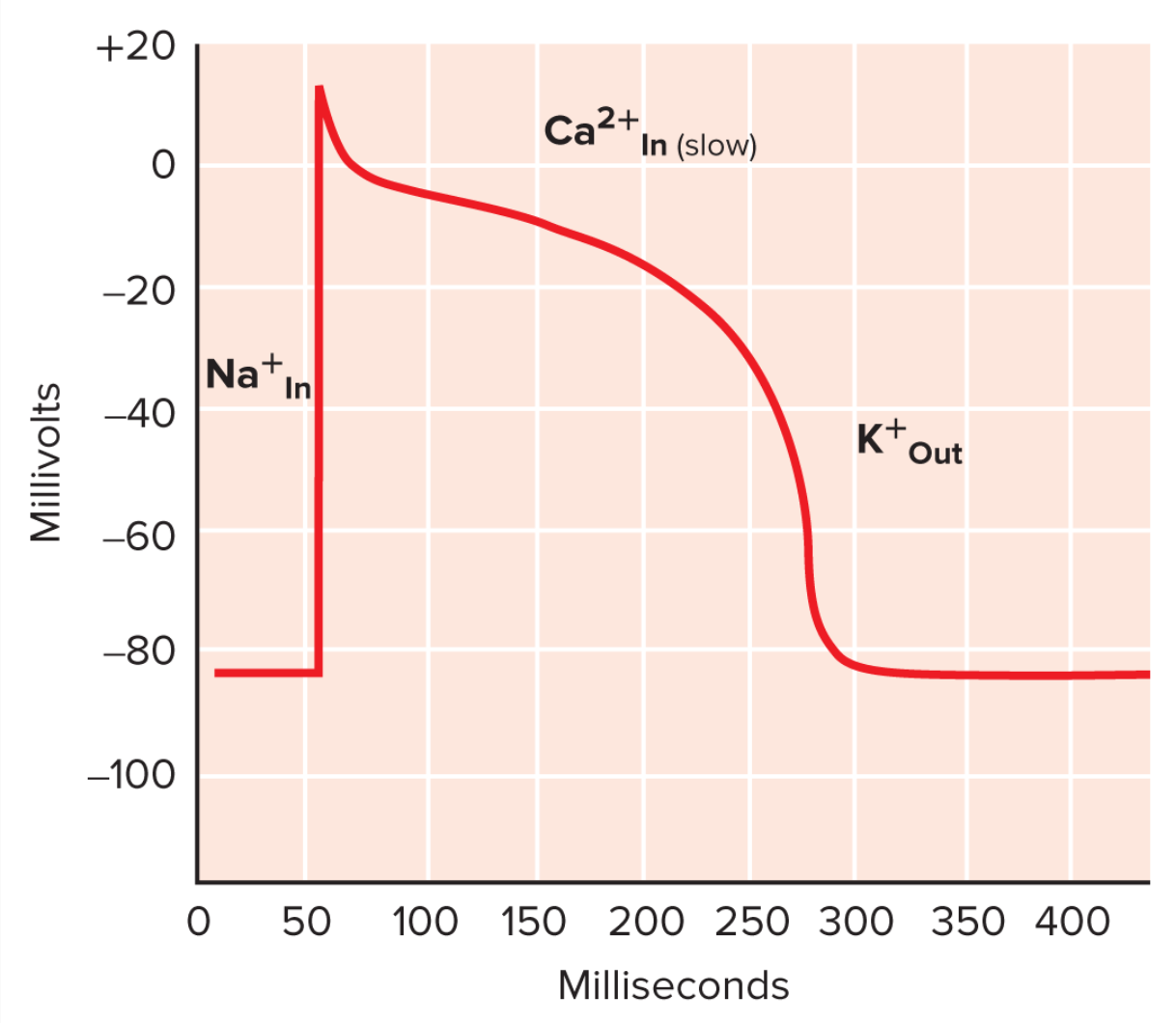
Action potentials originating in the SA node are conducted throughout the heart by the cardiac conduction system as described above. When a cardiomyocyte is stimulated by an action potential produced by the pacemaker region, it becomes depolarized and produces its own action potential. This depolarization causes voltage-gated sodium channels to open, allowing Na+ to rapidly enter the cell and increase the membrane potential of the cell.
Most action potentials in muscles are rapid (2-4 milliseconds) but action potentials in cardiac muscle can last up to 400 ms. The rapid influx of sodium activates voltage-gated calcium channels, causing calcium to begin entering the cell while potassium exits the cell. This phase of the action potential is known as the plateau phase, and is responsible for the S-T segment of an ECG (discussed below). After the plateau phase comes rapid repolarization, where the calcium channels close while potassium channels remain open. Potassium rapidly exits the cell, causing the membrane potential to return to its resting value of approximately -85 mV.
Action potentials in the cardiomyocytes enable muscle contraction by a process known as excitation-contraction coupling, common in both regular and cardiac muscle tissues. Calcium ions entering the cell during the plateau phase bind to and activate special ryanodine receptors in the sarcoplasmic reticulum of the cardiomyocytes, causing the sarcoplasmic reticulum to release stored calcium. This calcium release results in muscle contraction.
Electrocardiograms
Abbreviated EKG or ECG, an electrocardiogram is a depiction of the electrical conduction of the heart. It is taken by a machine known as an electrocardiograph. When an electrocardiogram is being taken with a traditional 12 lead electrocardiograph, 10 electrodes are placed on the limbs and chest of the person. This allows for the electrical conduction of the heart to be measured from 12 different perspectives. The machine is usually run for about 10 seconds. An EKG can help cardiologists diagnose cardiovascular disorders by detecting irregular heartbeat patterns (arrhythmias) and finding any possible areas of heart muscle damage. It may also be useful in monitoring the effects of certain medications.
Parts of an Electrocardiogram
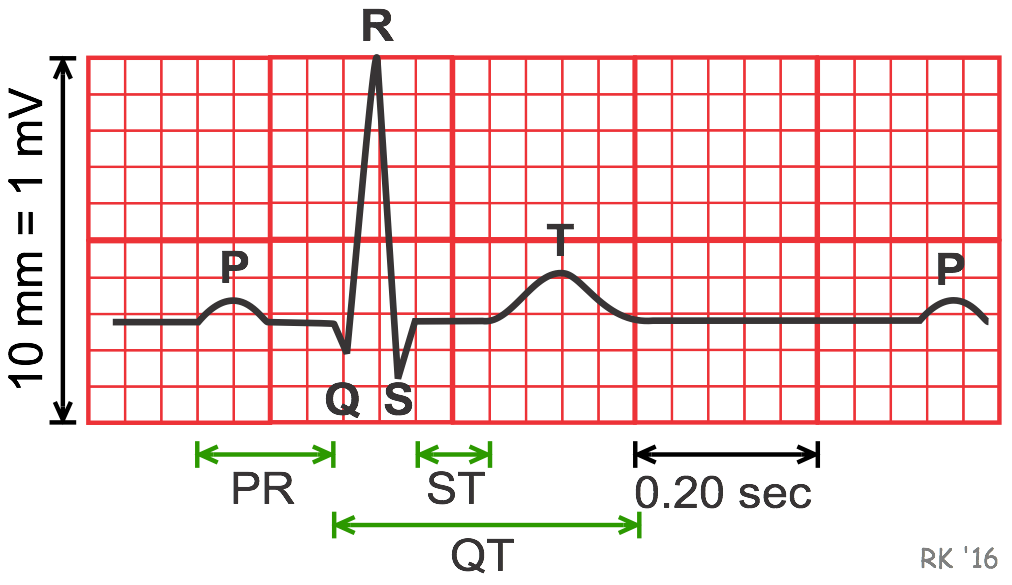
- P Wave: The P wave, shown by the first small bump in the electrocardiogram, marks the beginning of the heartbeat. When the electrical impulse is first sent from the sinoatrial node in the right atrium, it travels to the atrioventricular node and atrial muscle. The P wave is then generated by the activation of the muscle in the atria (atrial depolarization). Its duration should not be longer than .11 seconds.
- QRS Complex: The QRS complex is made up of the Q, R, and S waves, and is shown by a small peak below the baseline (Q wave), a large peak upward (R wave), and a peak slightly below the baseline again (S wave). After the electrical impulse reaches the AV node, it travels through the bundle of His, then the bundle branches, and then the Purkinje fibers to finally get to the ventricular muscle. When the septum is activated, the Q wave is generated. Next the ventricular free walls (both left and right) get activated, generating the R wave. Lastly, a few small areas which didn't get the electrical impulse before finally get it, generating the S wave. All in all, the QRS complex shows ventricular depolarization, and shouldn't last longer than .1 seconds.
- T Wave: The T wave is the last bump for one beat on an ECG. It should be larger than the bump that is the P wave. It indicates ventricular repolarization, or relaxation of the ventricles.
- ST Segment: The ST segment is the line between the S wave and the T wave. In a normal EKG, this segment should be mostly a straight line along the baseline. If the line goes up, or is elevated, more than 1mm, it indicates early ventricular repolarization, which is irregular and can lead to other cardiovascular problems.
- PR Interval: The PR interval is the time between the P wave and the R wave. It indicates the conduction time of the atrioventricular node, or the length of time it takes for the impulse to go through the AV node to the bundle of His. The normal duration time is .12 to .20 seconds.
- QT Interval: The QT Interval is the measure between the Q wave and the T wave. It measures the total time between ventricular depolarization and repolarization. The time for this measure is dependent on the heart rate, but the normal duration is .32-.4 seconds for a heart rate between 65-90bpm.
Mechanics of the Cardiac Cycle
The cardiac cycle refers to the sequences of events that occur in a single heartbeat. Blood flows due to pressure changes in the heart—the contraction of the muscle cells in the heart forces blood between chambers. Systole refers to contraction of the ventricles: both isovolumetric contraction and ejection are part of systole. The other phases (isovolumetric relaxation, rapid filling, and atrial contraction) are a part of diastole, which occur when the ventricles are relaxed. The heart pumps in two steps: both atria contract almost simultaneously before both ventricles contract almost simultaneously 0.1 to 0.2 seconds later. The entire cardiac cycle takes around 0.8 seconds at an average cardiac rate of 75 bpm. 0.5 seconds are spent in diastole, while the other 0.3 seconds are spent in systole.
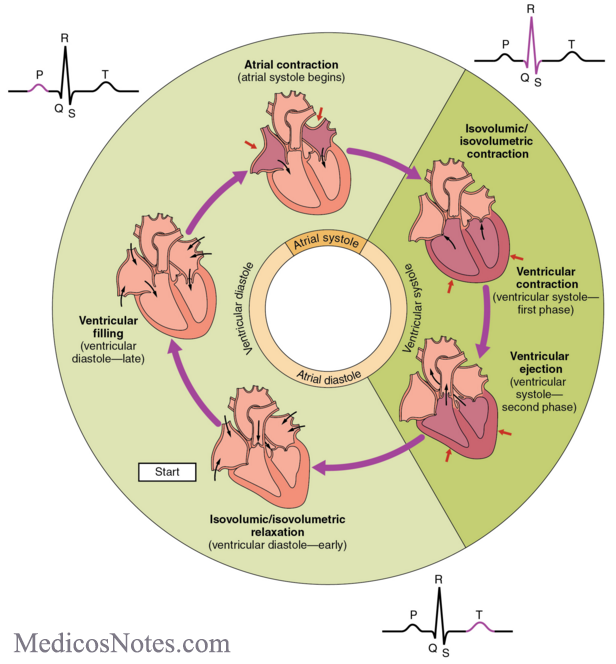
- Isovolumetric contraction: As the ventricles begin to contract, the pressure within them rises. This change in pressure causes the atrioventricular (mitral & tricuspid) valves to close, which produces the first "lub" heart sound. The pressure in the ventricles is not yet high enough to force the semilunar valves open, so both sets of valves are closed. No blood is able to enter or exit the ventricles, which is why this phase is called isovolumetric contraction: the volume remains the same throughout.
- Ejection: When the pressure in the left ventricle exceeds that of the aorta, the semilunar valves are forced open and ejection begins. Blood is forced out of the ventricles through the semilunar valves and into the aorta/pulmonary trunk. This phase is when systolic blood pressure is measured.
- Isovolumetric relaxation: As blood rushes out of the ventricles, the pressure within them decreases. When the pressure in the ventricles is lower than that of the arteries, the semilunar valves close. This is when the second "dub" heart sound is produced, as well as when diastolic blood pressure is measured. Both the semilunar and atrioventricular valves are closed during this phase as in isovolumetric contraction. During this phase, both the atria and ventricles are relaxed.
- Rapid filling: When the pressure within the ventricles falls below that of the atria, the atrioventricular valves open and rapid filling of the ventricles begins. Approximately 80% of the blood from the ventricles enters them due to gravity, while the other 20% is pushed into them during atrial contraction.
- Atrial contraction/atrial systole: The atria contract, pushing blood into the ventricles. After this the ventricles begin to contract, and the cardiac cycle begins anew.
Effect of Lifestyle on the Heart
This section is incomplete. |
Exercise
Many aspects of the heart change during exercise. It can help lower blood pressure, lessen the risk of diabetes, help maintain healthy body weight, and reduce inflammation throughout the body. It also improves the muscles of the heart and their ability to pull oxygen out of the blood. Furthermore, it reduces stress hormones that affect the heart and acts similarly to a beta-blocker to slow the heart rate (when not exercising) and lower the blood pressure. High-density lipoprotein levels are increased as well, and exercise can also help control triglycerides.
However, some bad things can happen too :( Too strenuous exercise keeps the body at a higher risk for Atrial fibrillation, CAD, and arrhythmia. As a result, people exercising should not try and go above their target heart rate.
Blood Vessels
Blood vessels form a network of tubes throughout the body which transport blood from the heart to the tissues and back again. Blood leaving the heart passes through vessels of increasingly small diameters, while blood returning to the heart passes through vessels of increasingly large diameters. There are three main types of blood vessels: arteries, veins, and capillaries.
- Arteries and Arterioles: These blood vessels carry blood away from the heart. For the most part, they carry oxygen rich, "red" blood, but there is one exception. The pulmonary arteries carry oxygen poor, "blue" blood away from the heart to the lungs. These vessels have very thick muscle cell layers since they need to pump the blood. Arteries are the vessels that lead immediately from the heart and other that lead from those. Arterioles are basically very small versions of arteries (20-30 µM in diameter), with much fewer muscle cells. They typically feed to the capillaries, though in some special cases they may feed into the venules.
- Elastic arteries are large arteries like the aorta which are rich in elastin fibers. These arteries will expand and recoil in response to changes in blood pressure, expanding under high pressure and recoiling under low pressure. Think of them as a rubber band snapping back into place when they are no longer stretched. The recoil force is responsible for pushing blood during the diastolic phase when the heart is resting.
- Muscular arteries are small arteries which have a thicker layer of muscle rather than elastin fibers. These arteries remain roughly the same diameter throughout the cardiac cycle and do not expand and recoil the same way elastic arteries do.
- Veins and venules: These blood vessels carry blood back to the heart from the rest of the body. For the most part, they carry oxygen poor, "blue" blood, but there is one exception. The pulmonary veins carry oxygen rich, "red" blood back to the heart from the lungs. These vessels have very small muscle layers and have valves. Venules are very small versions of veins. They directly take blood from the capillaries. Unlike arteries, they are low pressure and rely on contractions to carry blood back to the heart. Veins may also have valves which prevent backflow of blood.
- Capillaries: Capillaries are the smallest types of blood vessels (only 7-10 µM in diameter). It is in the capillaries that oxygen exchange and other exchanges of nutrients and wastes take place. Capillaries have a wall made of a single layer of epithelial cells, lacking the smooth muscle and elastic tissue present in veins and arteries. This allows materials to rapidly pass through the walls of the capillaries. Arterioles feed into capillaries and venules take used blood from them.
- Continuous capillaries have an uninterrupted lining of epithelial cells, only allowing small molecules like water to pass between the cells. These capillaries are found in locations like the muscles, lungs, and central nervous system.
- Discontinuous capillaries or sinusoidal capillaries are found in bone marrow, the liver, and the spleen. These capillaries have large gaps between the cells in the epithelial lining, producing an opening known as a sinusoid. This allows for large proteins to pass through easily.
- Fenestrated capillaries have large pores which allow materials to diffuse more rapidly. These are found in tissues like the kidneys, endocrine glands, and intestines. Unlike the sinusoidal capillaries, these capillaries have a membrane/diaphragm that stretches over the pores and regulates the passage of materials.
Structure
Veins and arteries are composed of three layers known as tunics.
- Tunica externa/tunica adventitia: The tunica adventitia is the outermost layer of the blood vessel and is entirely composed of connective tissue.
- Tunica media: The tunica media is the middle layer of the blood vessel, composed of smooth muscle and elastic fibers. This is what contracts when blood vessels constrict or dilate. Arteries generally have thicker tunica media than veins.
- Tunica interna: The tunica interna is the innermost layer of a blood vessel, consisting of three layers. The first is a simple squamous epithelium layer known as the endothelium which lines the interior of the blood vessel. A basement membrane connects the endothelium to a layer of subendothelial connective tissue, which is in turn linked to a layer of elastic fibers that form an internal elastic lamina.
Capillaries, being the smallest blood vessels, do not have all three layers. Instead, they are composed of a single layer of epithelial cells with an anchoring basement membrane. This allows for efficient diffusion of molecules out of the blood.
Blood
There are three main components of blood:
Red Blood Cells (Erythrocytes)- these blood cells are formed in the red bone marrow and are formed in the process of hematopoiesis (or more specifically, erythropoiesis). These cells lack a nucleus and are used to carry oxygen to the cells throughout the body. Each erythrocyte has a lifespan of about 120 days, and at the end of their lifespan, they are filtered out of the blood in the spleen. Erythrocytes also cannot reproduce. These cells contain hemoglobin- a protein that is used to allow the erythrocyte to carry oxygen. Each hemoglobin molecule can transport four molecules of oxygen, and there are about 250-270 million hemoglobin molecules in a single erythrocyte. Therefore, one erythrocyte can transport about 1-1.08 billion molecules of oxygen.
Platelets (Thrombocytes)- These blood cells are also formed in the red bone marrow and are formed in the process of hematopoiesis. These cells also do not contain a nucleus. These cells are produced from fragmentation of a larger precursor cell- the megakaryocyte. These cells help allow the blood to clot. Therefore this cell is necessary for the process of hemostasis- the process by which bleeding stops.

White Blood Cells (Leukocytes)- These blood cells are also formed in the red bone marrow and are formed in the process of hematopoiesis. Leukocytes help aid in the immune system. There are many different kinds of leukocytes, including: lymphocytes, basophils, neutrophils, eosinophils, monocyte, macrophage.
- Types of White Blood Cells
- Granulocytes - Granulocytes are white blood cells that have differently stained granules when viewed under a microscope. Granulocytes are Basophils, Neutrophils, and Eosinophils.
- Basophils - Basophils are a type of White Blood Cell, and more specifically a granulocyte. It is actually the least common white blood cell in the body. They are thought to be associated with allergies, as they can secrete a substance known as histamine.
- Agranuloctyes - Agranulocytes are white blood cells that lack visible granules in the cytoplasm and have spherical or ovoid nuclei. Agranulocytes are Lymphocytes and Monocytes.
- Lymphoctyes - Lymphyoctyes makeup about 25% of all white blood cells in the blood (2nd most numerous) and are often found in lymphatic tissue. They contain a large, purple staining nucleus that takes up most of the volume of the cell.
- Monocytes - These white blood cells are less common, making up only around 3-8% of the total amount of white blood cells in the blood. They are the one of the largest cells in the body and contain a U-shaped nucleus.
- Granulocytes - Granulocytes are white blood cells that have differently stained granules when viewed under a microscope. Granulocytes are Basophils, Neutrophils, and Eosinophils.
Hematopoiesis
Hematopoiesis is the process by which all blood cells (erythrocytes, thrombocytes, and leukocytes) are made. All the blood cells start out as a stem cell. Then the stem cell specializes to eventually become one of the types of blood cells.
Coagulation
This section is incomplete. |
When the blood vessels are injured, the body has several steps it can take to stop bleeding (undergo hemostasis). The most important of these is coagulation, or blood clotting. Blood clotting is the conversion of a soluble protein (fibrinogen) to an insoluble protein (fibrin) which forms a mesh that makes up a majority of the blood clot. There are two blood clotting pathways: intrinsic and extrinsic. Ordinarily, blood left outside of the body (e.g. in a test tube) will clot on its own. This occurs via the intrinsic pathway. The extrinsic pathway is faster than the intrinsic pathway, but it requires the release of a tissue factor produced by damaged tissues to take place. This means it cannot occur outside the body.
Blood clots are composed of fibrin as well as platelets. Ordinarily, platelets are repelled from the walls of the blood vessel by the endothelial lining. Connective tissues and collagen deeper in the blood vessel are capable of binding to platelets when exposed, causing them to accumulate. von Willebrand's factor (VWF) binds to the platelets and collagen, anchoring them and preventing them from being swept away by the flow of blood. When a platelet is bound to collagen in the blood vessel, it begins to release its contents (degranulate) in a process known as the platelet release reaction. This makes them "sticky", allowing more platelets to bind and degranulate. This produces a platelet plug which forms the base of a blood clot.
The platelet release reaction also activates clotting factors found in the plasma. These clotting factors help catalyze the conversion of fibrin to fibrinogen. One clotting factor activates another until thrombin converts fibrinogen to fibrin.
Cardiovascular System Disorders
| Disease Name | Cause | Symptoms | Treatment | Prevention | Effect on the Body |
|---|---|---|---|---|---|
| Atherosclerosis/Arteriosclerosis | Smoking, High Blood Cholesterol, Hypertension, Build up of plaque in the arteries | Normally asymptomatic, if in the coronary arteries- angina, shortness of breath, arrhythmia | Lifestyle changes- quit smoking, eat healthier, exercise, lose weight, reduce stress. Angioplasty, Coronary Artery Bypass Grafting | Control risk factors, know family history of atherosclerosis | Hardening of arteries due to either age or the build up of plaque in the arteries |
| Hypertension | Risk factors, age, medical problems, bad diet, obesity, gender, smoking | Usually asymptomatic, headaches if serious, people learn after complications start | Lifestyle changes, Medicines- diuretics, beta blockers, ACE inhibitors, Alpha blockers | Control risk factors, medicines | High blood pressure, damage to internal organs |
| High Blood Cholesterol (Hypercholesterolemia) | Diet, weight, activity, heredity, age/sex | Asymptomatic | Control risk factors/ make lifestyle changes, medications- statins, bile acid sequestrants, fibrates | Control Risk factors | Too much cholesterol in blood. Cholesterol is in plaque. Low Density Lipoprotein (LDL) is the "bad" cholesterol, and High Density Lipoprotein (HDL) is the "good" cholesterol |
| Stroke | Obstructed blood flow to brain, 2 types- ischemic- too little blood, Hemorrhagic stroke- too much blood in skull | Trouble walking, speaking. Paralysis/numbness on 1 side of body, trouble seeing, headache, a Transient Ischemic Attack (a temporary lack of blood to the brain) | Control risk factors, restore blood flow, aspirin, Tissue plasminogen activator, angioplasty | Control risk factors, anti-platelet drugs, anticoagulants | Blood flow blocked to brain, death of brain tissue |
| Heart Attack (Myocardial Infarction) | Build up of plaque in coronary arteries, blocking of blood flow to heart, spasm | Chest pain- pressure/squeezing/fullness, arm/jaw/back pain, shortness of breath | Aspirin, Nitroglycerin, Thrombolytic Meds, Beta Blockers, ACE Inhibitors, Anticoagulants, Angioplasty, Coronary Artery Bypass Grafting | Control Risk Factors for heart disease | Blood flow obstructed to heart, death of heart tissue |
| Cardiogenic Shock | Heart attack, other heart conditions | Confusion, lack of alertness, loss of consciousness, rapid heart beat, seating, weak pulse, cold at touch | Emergency life support, medicines to help the heart, angioplasty/stents, Coronary Artery Bypass Grafting, other surgeries | Control risk factors for heart disease, get help immediately if you have a heart attack | The weakened heart isn’t able to pump enough blood to the body |
| Lymphoma | Not known | Swollen lymph nodes, fatigue, weakness, weight loss, fevers | Radiation, Chemotherapy | Stop smoking, not much you can do to control | Cancer of the immune system- lymphocytes |
| Kawasaki's Disease | Thought to be a response to a virus | Swollen lymph nodes, rash, red lips, red palms, redness of eyes, joint pain | Aspirin, prevent from getting to coronary vessels, surgical treatment rare | No prevention | Inflammation of blood vessels- can effect any vessels |
| Atrial Fibrillation | Electrical signals in heart are abnormal | Palpitations, Shortness of breath, weakness, chest pain, fatigue | Prevent clots, aspirin, Rhythm Control | Healthy Lifestyle | Abnormal heart electrical conduction, can cause complications |
| Congestive Heart Failure | Coronary Artery Disease, hypertension, arrhythmias, heart muscle diseases | Shortness of breath, swelling in ankles, feet, abdomen, legs, fatigue | Treat underlying cause, lifestyle management, medicines- ACE inhibitors, beta blockers, diuretics
Artificial pacemaker, implanted defibrillator, heart transplant |
Control risk factors for heart diseases | When the body cannot pump enough blood to the rest of the body. |
Disorders Mentioned in Rules
This page is outdated. |
Congestive Heart Failure:
- General Overview: AKA heart failure, CHF is the leading cause of hospitalization in people over 65, in which the heart is unable to pump properly. Left CHF is more common than right. In systolic left CHF, the left ventricle cannot contract normally, and reduces force that blood is being pushed out. In diastolic left CHF, the left ventricle stiffens and cannot relax, which prevents heart from filling with blood in between beats. Right CHF usually occurs when left CHF spreads from being untreated, and causes fluid to get into the lungs. Four classes of CHF: 1 (experiencing no symptoms during physical activity), 2 (physical activity causes fatigue, palpitations, shortness of breath), 3 (mild exercise causes symptoms very quickly), 4 (no physical activity can be done without facing symptoms).
- Causes: Hypertension can cause heart muscle to become thicker and overworked, eventually causing the muscle to not work as well. Coronary Artery Disease limits blood flow to the heart muscle, causing it to not work as well as it should. Valves that don’t work correctly force ventricles to work harder to pump blood.
- Diagnosis: Blood tests, EKG, Chest X-ray, Echocardiogram, Exercise (stress) test, cardiac catheterization, MRI.
- Symptoms: Early: fatigue, swelling of legs, ankles, and feet, weight gain, increased urination need. Mid: irregular heartbeat, cough from lungs, wheezing, shortness of breath (indicates pulmonary edema). Late: chest pain, rapid breathing, blue skin, fainting.
- Treatment: No cure, treatment of symptoms through heart healthy diet, and exercising. Medications include ACE inhibitors, Beta blockers, diuretics, angioplasty, valve repair surgery.
Atrial Fibrillation:
- General Overview: AKA arrhythmia, is an irregular heartbeat that is caused by the electrical system of the heart not functioning properly. It increases risk of stroke and heart disease. It can cause blood to pool up in the atria because the atria and ventricles are not contracting in the pattern they’re supposed to.
- Causes: Age, genetics, heart disease, hypertension, COPD, emphysema, pulmonary embolism, sick sinus syndrome.
- Diagnosis: Cardiologists may listen to heartbeat to get pulse and rhythm, may listen to lungs, and check for signs of heart valve or heart muscle problems. An EKG will be taken and a Holter monitor might be placed for a day or two.
- Symptoms: Fatigue, irregular heartbeat, fluttering or “thumping” in chest, dizziness, shortness of breath, anxiety, chest pain (indicative of heart attack), chest pressure, sweating, fatigue, weakness, excessive sweating.
- Treatment: Blood thinners, rate controllers, rhythm controllers, anticoagulants, beta blockers, calcium channel blockers, digoxin, sodium channel blockers, potassium channel blockers, electrical cardioversion (like AED), ablation, pacemaker, open heart maze procedure.
Myocardial Infarction (Heart Attack):
- General Overview: AKA heart attack, a myocardial infarction is the death of heart muscle due to the muscle not getting enough oxygen. Heart attacks usually occur over the span of several hours. Heart attacks are usually preceded by anginas, which are brief periods of chest pain.
- Causes: Coronary artery disease is the main cause of a heart attack, for it blocks the blood flow to the muscle of the heart, causing it to die. Risks include hypertension, high cholesterol levels, obesity, smoking, genetic history, and sedentary lifestyle.
- Diagnosis: Diagnosis is done through an EKG, which can also help determine which areas of cardiac muscle were affected by the heart attack.
- Symptoms: Discomfort in chest, arms, or breastbone area, choking feeling, sweating, nausea, rapid/irregular heartbeat, shortness of breath, dizziness.
- Treatment: Aspirin, to prevent blood clotting, other antiplatelets, angioplasties or insertion of stents may be done to prevent another one from occurring.
Atherosclerosis:
- General Overview: Clogging of arteries due to the buildup of fats (cholesterol), and narrows the blood vessels. It is the most common cause of cardiovascular disease.
- Causes: Begins with cholesterol or hypertension damaging endothelium of arteries. LDL cholesterol gathers to form plaque, narrowing and hardening arteries. People have a higher risk if they have hypertension, high LDL cholesterol levels, and smoking.
- Diagnosis: Angiogram is done to determine sites of blockage.
- Symptoms: None when starting off, start to occur after plaque ruptures or blockage is so severe as to block blood flow. When they do occur, commonly there will be pain in legs or chest when exerting.
- Treatment: Stents, angioplasty, coronary bypass surgery, blood thinners, cholesterol medication (statins), heart-healthy diet, more exercise, weight loss.
Bradycardia:
- General Overview: Low heart rate, characterized under 60 bpm at rest. Occasionally, having bradycardia will not mean anything, as it might be natural. Bradycardia is diagnosed only when symptoms are present.
- Causes: May be caused as a result of the heart’s electrical system not functioning properly. Factors that increase risk include smoking, drug abuse, hypertension, thyroid disease, and some medications like beta blockers.
- Diagnosis: EKG will be done and heart monitor may be put on for 24 hours.
- Symptoms: Dizziness, shortness of breath, fainting, confusion, fatigue, weak pulse.
- Treatment: Treatment is based on cause, so if hypothyroidism is the cause, then they’ll treat for hypothyroidism. Pacemaker may also be inserted to set normal rhythm of heart.
Tachycardia:
- General Overview: Type of arrhythmia in which heart beats faster than normal while at rest, characterized with over 100 bpm. Three types: supraventricular, ventricular, and sinus tachycardia. In supraventricular, electrical signals in atria misfire, causing heart rate to speed up, which prevents blood from filling the chambers and leads to decreased flow of blood to body. Ventricular is similar, except misfiring occurs in ventricles, which still leads to decreased flow of blood to body. In sinus tachycardia, SA node sends out signals faster than normal, but flow of blood is normal.
- Causes: Sinus tachycardia can be caused by strenuous exercise, anxiety, fever, fear, stress, certain medications, street drugs, anemia, hyperthyroidism, or heart failure. Supraventricular affects those that smoke, drink, or have a lot of caffeine. Ventricular occurs with lack of oxygen, sarcoidosis, electrolyte imbalance, cardiomyopathy, or some medications.
- Diagnosis: Tests like EKG, exercise stress tests, or magnetic source imaging may be done.
- Symptoms: Dizziness, lightheadedness, shortness of breath, fainting, heart palpitations, chest pain, rapid pulse. Sometimes, people are asymptomatic.
- Treatment: Less caffeine and alcohol consumption, quit smoking, fibrillator (reset electrical system).

